Introductory Materials
Athletic Training Milestones Project
The Athletic Training Milestones Project Team has worked collaboratively since 2016 to develop the Athletic Training (AT) Milestones to enhance and facilitate assessment of student and resident learning. The AT Milestones are designed for use in evaluation of athletic trainers in the context of their participation in Commission on Accreditation of Athletic Training Education (CAATE) accredited professional education, residency, and fellowship programs.


The Value of Athletic Trainers in Ambulatory Settings
Frogner BK, Westerman B, DiPietro L
Athletic trainers (ATs) are increasingly used in ambulatory care settings. This study piloted a new survey instrument to assess the value that ATs add to these settings. The survey collected data on six domains: 1) general facility characteristics, 2) AT staffing characteristics, 3) other staffing characteristics, 4) patient characteristics, 5) billing practices, and 6) participation in innovations. A national sample of physician practices using ATs was recruited to participate in a web-based survey. The study found that ATs were among the most common clinical occupations in the practice. Practices were almost all "very satisfied" with the services provided by ATs with equal expectations to either maintain or increase the number of ATs. While most practices invested in training and continuing education units, the larger practices were more likely to do so. Practices were more likely to bill for AT services if ATs had a national provider identifier. The mean number of clinical visits, rate of billing, patient scheduling, wait times, and participation in innovations did not vary significantly by the number of ATs employed. Overall, the study found evidence that ambulatory care practices see value in hiring ATs.
Hiring Patterns of Athletic Trainers in Ambulatory Care Settings
Frogner BK, Westerman B, DiPietro L
Athletic trainers (ATs) are often employed to provide direct patient care in ambulatory care settings, particularly in orthopedic practices. Given their training, ATs may both complement and substitute for services otherwise delivered by physicians or other providers such as physician assistants (PAs) and nurse practitioners (NPs). With concerns about projected primary care provider shortages,1 ATs may be hired to deliver cost-effective ambulatory care practices and to help keep up with the growing demand for primary care. The value of ATs in ambulatory care practices, however, is not widely recognized, in part due to the limited amount of research on the role of ATs in these settings.
This study aims to add to the literature by identifying the motivations of ambulatory care practice administrators for hiring an AT, and to gauge the perceived value of ATs in ambulatory care settings. In our expert interviews, we learned that ambulatory care practice administrators were satisfied with the work of ATs and that they planned to maintain or increase the number of ATs working in their practices. The respondents placed a high value on the knowledge and skills of the ATs they employ. While a larger study is necessary to track and assess the role of ATs in ambulatory care practices, the findings of our study highlight the value and potential growth in the demand for ATs for delivering patient care in ambulatory care settings
Athletic Trainers Pump up Care in Orthopedics Clinic
An editorial by Tyler Smith
The words “athletic trainer” might conjure images of hard-core sports enthusiasts of the professional or weekend warrior variety, sweating through rehab regimens to get their joints in shape so they can hit the fields or the slopes once more. The picture is not untrue, but it is incomplete. In the wider world, certified athletic trainers (ATCs) can help people recovering from orthopedic procedures get back to no-less-important activities, like gardening, walking the dog, or wrestling with the kids.
Using Athletic Trainers with Mid-Level Providers to Add Clinical and Financial Value to a Practice
An editorial by Joe J Greene
As orthopaedic and sports medicine practices evolve and react to the challenges they face driven by national health care policy change and diminishing reimbursement, they are forced to consistently evaluate their processes and find ways to deliver care more efficiently and effectively. If done well, this evolution occurs while adding clinical value to the patient while simultaneously adding financial value to the practice.
5 Tips for Promoting Efficiency at Orthopedic Practices
An editorial by Laura Dyrda
Here are five ways to ensure your orthopedic practice is running efficiently.


Comparison of the Effect of Medical Assistants Versus Certified Athletic Trainers on Patient Volumes
Pecha FQ, Xerogeanes JW, Karas SG, Himes ME, Mines BA
Research has shown increases in efficiency and productivity by using physician extenders (PEs) in medical practices. Certified athletic trainers (ATCs) that work as PEs in primary care sports medicine and orthopaedic practices improve clinic efficiency.
Hypothesis: When compared with a medical assistant (MA), the use of an ATC as a PE in a primary care sports medicine practice will result in an increase in patient volume, charges, and collections.
Conclusion: ATCs can optimize orthopaedic sports medicine practice by increasing patient encounters, charges, and collections.
Athletic trainers can move from the playing field into the office as physician extenders
Insight by Marjorie J. Albohm and John W. Xerogeanes, MD
More orthopedists are looking to employ athletic trainers as physician extenders to increase practice efficiency, revenue and productivity, while ensuring patient education and satisfaction.“To some orthopedists, it is new and different,” John W. Xerogeanes, MD, chief of the Emory Sports Medicine Center, told Orthopedics Today. “It can be a big improvement compared to what we have in terms of quality of care, and you can also significantly save on the financial side.”
Athletic Trainers in an Orthopedic Practice
Greene JJ
Athletic Trainers at the University of Wisconsin Hospital have assisted orthopedic and primary-care sports-medicine physicians in the clinic since 1981. At the core of our success is the long-standing relationship of the certified athletic trainer and the team physician. We have extended the traditional on-the-field athletic training room model to the sports-medicine orthopedic clinic. This model has produced excellent clinic efficiency and flow and increased revenue for our hospital and physicians. Presently, the UW Health Sports Medicine Clinic has eight sportsmedicine-fellowship-trained physicians. Four of these have specialties in orthopedics, two in family medicine, and two in pediatrics. They are also the team physicians for the University of Wisconsin Athletic Department. A total of a 4.0 FTE equivalent of athletic trainers staff these clinics along with nurses, physician assistants, medical assistant, residents, and fellows. The athletic trainers are all hospital employees and are not employed by the physician group. The responsibilities of the various support staff are described in the sidebar.
Certified Athletic Trainers An Evaluation of Their Effect on Patient Throughput & Revenue Generation
Pecha FQ, Karas SG, Xerogeanes JW, Dougherty T, Mines BA, Labib S, Kane A
While medical assistants (MAs), physician assistants (PAs) and nurses (RNs) are the “typical” clinical assistants used in physician practices, certified athletic trainers (ATs) — highly educated health care professionals who specialize in the prevention, assessment and rehabilitation of musculoskeletal injuries and illnesses — are gaining recognition as unique, skilled and valuable health care professionals in orthopaedic offices. In an effort to evaluate the benefit of employing certified athletic trainer, Emory Sports Medicine Center implemented a study to determine the financial and clinical effectiveness of using them as the primary clinical assistant in the orthopaedic office. By comparing the number of patient encounters and financials (bill charges and collections) of two primary care physician practices — both before and during the introduction of a certified athletic trainer — it was shown that certified athletic trainers had a positive effect on patient throughput and revenue. Results showed that ATs can increase a physician’s productivity up to 23% and increase revenue by up to 42%.
A New Twist: Using Certified Athletic Trainers as Physician Extenders
Holm L
A new health care model has evolved that uses certified athletic trainers (ATCs) as physician extenders. ATC's commpliment the work of other health care professionals such as physician assistants (PAs), nurse practitioners (NPs) and physical therapists (PTs).
Education Continues to Evolve: Post-Professional Work Expands
An editorial by Valerie Hunt


Adding Athletic Trainers to Care Team Can Increase Docs' Productivity
An editorial by David Mitchell
According to the National Athletic Trainers' Association, or NATA, nearly 8,000 of its members worked in hospitals, clinics and physician offices last year (2003), and the number is growing. That figure, which represents more than a quarter of the association's members, is up more than 4 percent since 2001. The services these health professionals provide can bring significant value to a medical practice, says one family physician.
The Athletic Trainer as Orthopedic Physician Extender
An editorial by John W. Xerogeanes, MD
Supply and demand are the primary factors that drive our capitalistic economy. Professional opportunities and monetary compensation in a free market society are primarily determined by these factors. No matter how talented and highly skilled a particular group of professionals may be, success in the marketplace depends upon the specific needs of consumers and employers and possession of the specific professional capabilities to fulfill that demand. Between the two worlds of orthopedic surgery and athletic training, we have both the need and the skill to form a symbiotic working relationship. What we have been missing is a reproducible mechanism to bring the two together in a more integrated manner. In the last issue, Forrest Pecha’s editorial promoted the Orthopedic Athletic Training Fellowship concept as a valuable educational experience for athletic trainers. I will try to expand on his message from the perspective of an orthopedic surgeon.
Practice Profiles: Athletic Trainers in Orthopedic Offices
Featuring Aaron Hajart, Bryan Diekmann, Forrest Pecha and Mike Doyle
Athletic trainers (ATs) are routinely employed in hospitals, clinics, and in sports medicine, family, pediatric, orthopedic and physiatry practices. Physicians and practice managers say ATs working in these settings improve physician productivity, patient outcomes and satisfaction. They move patients more effectively and efficiently through the appointment and treatment process. By treating more patients in the same period of time, physicians are able to improve patient access, throughput and revenue generation
Marketing Athletic Trainers to Sports Medicine Physicians
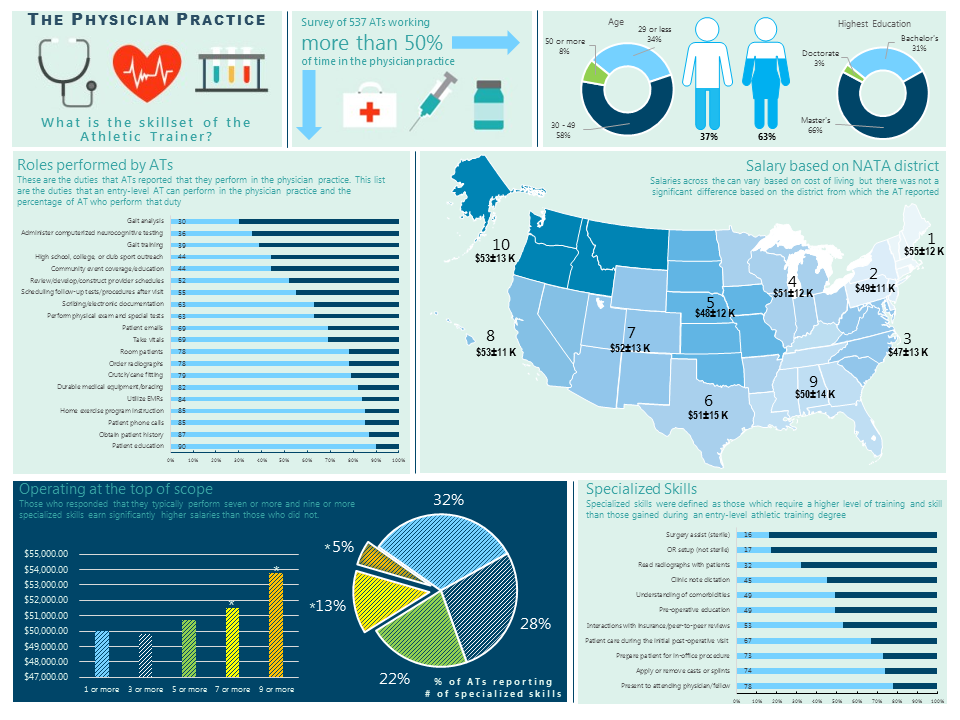
Infographic